Smoking Out the Therapeutic Possibilities of Cannabinoids
- Published20 Apr 2017
- Reviewed20 Apr 2017
- Author Teal Burrell
- Source BrainFacts/SfN
Desperate for relief from unrelenting chronic pain, many people turn to marijuana. As of November 2016, 28 states and the District of Columbia have legalized some form of medical marijuana for chronic pain and other conditions, such as seizures and migraines.
Proponents of medical marijuana point to the drug’s history: it’s been used as a medicine for thousands of years and has never been shown to cause death from an overdose. Many doctors, particularly oncologists, support legalizing marijuana for nausea, loss of appetite, pain, and depression in cancer patients.
Even so, the federal government has not approved of the marijuana plant for any conditions, citing a lack of evidence of its benefits. In the U.S., marijuana is classified as a Schedule I drug, a designation for drugs deemed to have no medical use and a high potential for abuse. The Schedule 1 classification also restricts how government-funded labs can study marijuana, meaning such research is difficult to perform. At the same time, the government will only lift the restrictions if federally-funded researchers and institutions can provide ample evidence of marijuana’s therapeutic potential — a catch-22. “The regulation makes studying the plant and its components extremely tricky,” says neurobiologist Margaret Haney, director of Columbia University’s Marijuana Research Laboratory.
To get around the restrictions, some scientists are investigating an alternative: the marijuana-like compounds produced naturally in the brain. The compounds, called endocannabinoids, act on brain cells in the same way as the cannabinoid chemicals in marijuana, binding to receptors on neurons and changing how the cells behave. Endocannabinoids help regulate pain, appetite, and anxiety. Manipulating them — by enhancing their activity or by administering synthetic versions of the chemicals — may provide similar benefits to marijuana and may represent a more viable way to treat conditions like post-traumatic stress disorder and chronic pain.
Less Anxiety
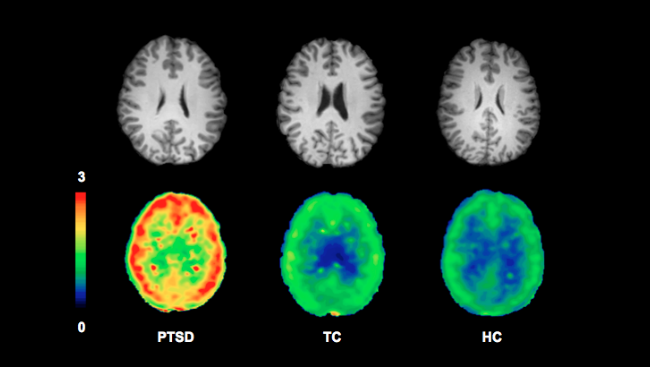
Many combat veterans turn to marijuana to help ease the intense fear, anxiety, and flashbacks associated with post-traumatic stress disorder, or PTSD. It turns out, marijuana might offer some relief by restoring normal brain chemistry. Not everyone exposed to trauma goes on to develop PTSD, but those who do have lower levels of a natural cannabinoid, anandamide, in their brains, raising the possibility that marijuana might normalize cannabinoid signaling. People living with PTSD may also have more inflammation in their brains, and cannabinoids have been shown to have anti-inflammatory properties as well as a role in diminishing fear memories.
Sabrina Lisboa at the University of São Paulo in Brazil tested whether a synthetic cannabinoid could diminish fear memories and inflammation in stressed mice. After receiving either the cannabinoid or a placebo, the mice were placed in a stressful situation — being bullied by an aggressive, dominant mouse — every day for six days. Next, Lisboa put the mice in a cage that had previously delivered a foot shock. Mice that received the placebo continued to freeze in fear when put in this cage, even long after the shocks stopped, a behavior reminiscent of the unrelenting fear people with PTSD experience after trauma. Mice that received the synthetic cannabinoid, on the other hand, quickly learned the cage was now harmless and stopped freezing. These mice also had lower levels of inflammation in the frontal cortex and hippocampus, areas of the brain implicated in PTSD.
Part of the resistance to medical marijuana stems from concern about potential side effects like paranoia, memory problems, and impaired motor coordination. Lisboa’s work suggests isolating marijuana’s active chemicals, rather than using the entire plant, may be a way to relieve some symptoms of PTSD while minimizing the potential risks.
Less Pain
Still, flooding the body with isolated cannabinoids could produce undesired effects very similar to marijuana. As an alternative, some scientists are looking for ways to augment the marijuana-like chemicals already in the brain.
When the natural chemicals — endocannabinoids — bind to protein receptors on neurons, they unleash a wave of molecular events that changes how the neurons behave. In the case of the cannabinoid 1, or CB1, receptor, the result is pain relief.
Andrea Hohmann of Indiana University wanted to find a way to enhance this natural pain relief, so she investigated a molecule that helps endocannabinoids link up with CB1 receptors. Positive allosteric modulators, or PAMs, are a type of molecule that increases the odds a signaling molecule will find its receptor or helps the two form a stronger connection. Hohmann selected a PAM known to bind to the CB1 receptor and promote endocannabinoid activity. Mice given a drug that causes nerve damage were hypersensitive to pain, but mice that receive the PAM in addition to the drug had a normal tolerance for pain. And, compared to other experiments using marijuana or cannabinoids, the mice displayed fewer side effects and they didn’t show signs of becoming addicted, like tolerance or withdrawal. But in places or at times when endocannabinoids are not normally present, the PAM will have no effect.
“An advantage of the positive allosteric modulator would be that we would only be boosting endocannabinoid signaling under conditions in which it’s already being released,” Hohmann says. If endocannabinoids are not normally present, the PAM will have no effect.
Chronic pain affects nearly 50 million Americans, and opioids — the gold standard of analgesics — are fraught with risks including abuse, overdose, and death. Hohmann hopes the PAM could one day be an alternative to prescription opioids.
More Research
Neuroscientists are just beginning to discover the potential of manipulating the endocannabinoid system, and could find it has benefits beyond treating PTSD and chronic pain. But, like the effects of marijuana, more research is needed. “Our scientific understanding of the therapeutic potential of the marijuana plant is really in its infancy, as is our understanding of the THC-like chemicals in our brain and their potential therapeutic use,” says Haney. “What’s exciting is all these other compounds, and we’re just starting to really learn about them.”
CONTENT PROVIDED BY
BrainFacts/SfN
References
Clapper J. Researchers develop novel compound that alleviates chronic pain symptoms in rats. Press conference at the annual meeting of the Society for Neuroscience (2016).
Hohmann A. Amplifying endocannabinoid signaling decreases pain behaviors in mice. Press conference at the annual meeting of the Society for Neuroscience (2016).
Klein T. Cannabinoid-based drugs as anti-inflammatory therapeutics. Nature Reviews Immunology, 5: 400-411 (2005).
Lisboa S. A synthetic cannabinoid reduces anxiety and inflammation in stressed mice. Press conference at the annual meeting of the Society for Neuroscience (2016).
Michopoulous V, Powers A, Gillespie C, et al. Inflammation in Fear- and Anxiety-Based Disorders: PTSD, GAD, and Beyond. Neuropsychopharmacology,
National Academies of Sciences, Engineering, and Medicine. The health effects of cannabis and cannabinoids: Current state of evidence and recommendations for research (2017).
Neumeister A, Normandin M, Pietrzak R, et al. Elevated brain cannabinoid CB1 receptor availability in post-traumatic stress disorder: a positron emission tomography study. Molecular Psychiatry, 18: 1034-1040 (2013).


















