Touch and Pain
- Published1 Apr 2012
- Reviewed1 Apr 2012
- Source BrainFacts/SfN
Touch is the sense by which we determine the characteristics of objects: size, shape, and texture.
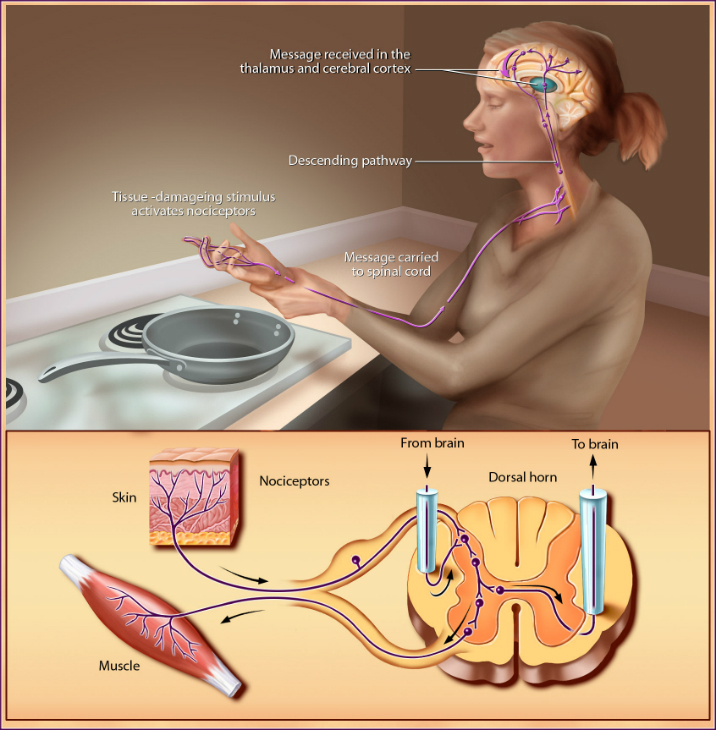
Pain messages are picked up by receptors and transmitted to the spinal cord via small myelinated fibers and very small unmyelinated fibers. From the spinal cord, the impulses are carried to the brainstem, thalamus, and cerebral cortex and ultimately perceived as pain. These messages can be suppressed by a system of neurons that originates in the midbrain. This descending pathway sends messages to the spinal cord where it suppresses the transmission of tissue damage signals to the higher brain centers.
We do this through touch receptors in the skin. In hairy skin areas, some receptors consist of webs of sensory nerve cell endings wrapped around the base of hairs. The nerve endings are remarkably sensitive. They can be triggered by the slightest movement of the hairs.
Signals from touch receptors pass via sensory nerves to the spinal cord, where they synapse, or make contact with, other nerve cells, which in turn send the information to the thalamus and sensory cortex. The transmission of this information is highly topographic, meaning that the body is represented in an orderly fashion at different levels of the nervous system. Larger areas of the cortex are devoted to sensations from the hands and lips; much smaller cortical regions represent less sensitive parts of the body.
Different parts of the body vary in their sensitivity to tactile and painful stimuli. These varying responses are based largely on the number and distribution of receptors. For example, the cornea is several hundred times more sensitive to painful stimuli than are the soles of the feet. The fingertips are good at touch discrimination, but the torso is not.
Neurologists measure sensitivity by determining the patient’s two-point threshold, the distance between two points on the skin necessary in order for the individual to distinguish two distinct stimuli from just one. This method involves touching the skin with calipers at two points. Not surprisingly, acuity is greatest in the most densely nerve-packed areas of the body. The threshold is lowest on the fingers and lips.
The sensory fibers that respond to stimuli that damage tissue and can cause pain are called nociceptors. Different nociceptor subsets produce molecules that are responsible for the response to noxious (i.e., painful) thermal, mechanical, or chemical stimulation. Interestingly, these same molecules respond to plant-derived chemicals, such as capsaicin, garlic, and wasabi, that can produce pain. Some nociceptors in the skin respond to chemical stimuli that cause itch. Histamine is an example of such a nociceptor, and it can be released in response to certain bug bites or allergies.
Tissue injury also causes the release of numerous chemicals at the site of damage and inflammation. Prostaglandins enhance the sensitivity of receptors to tissue damage and ultimately can induce more intense pain sensations. Prostaglandins also contribute to the clinical condition of allodynia, in which innocuous stimuli can produce pain, as when sunburned skin is touched.
Persistent injury can lead to changes in the nervous system that amplify and prolong the “pain” signal. The result is a state of hypersensitivity in which pain persists and can even be evoked by normally innocuous stimuli. Persistent pain is in many respects a disease of the nervous system, not merely a symptom of some other disease process.
CONTENT PROVIDED BY
BrainFacts/SfN