Gambling Addiction and the Brain
- Published3 Sep 2015
- Reviewed3 Sep 2015
- Author Mary Bates
- Source BrainFacts/SfN
Gambling — whether it be the lottery, scratch cards, casino games, bingo, slot machines, Internet poker, or sports betting — is more acceptable and accessible than ever before. For most people, gambling is a recreational activity. But for a significant minority, it progresses to a serious problem.
Recently, scientists and mental health professionals decided to classify problem gambling as a behavioral addiction, the first of its kind, putting it in a category of disorders that also includes substance abuse. The reason for this change comes from neuroscience research, which has shown that gambling addicts have a lot in common with drug and alcohol addicts, including changes in behavior and brain activity.
A Behavioral Addiction
Gambling disorder refers to the uncontrollable urge to gamble, despite serious personal consequences. Problem gambling can impact a person's interpersonal relationships, financial situation, and physical and mental health. Yet it has only recently been recognized as an addiction.
Problem gambling was first classified as a psychiatric disorder in 1980. In the third edition of the Diagnostic and Statistical Manual, the American Psychiatric Association's guide to psychiatric disorders, the condition was termed "pathological gambling" and classified as an impulse control disorder, alongside disorders like kleptomania and pyromania. In 2013, it was renamed "gambling disorder" and moved to the Substance-Related and Addictive Disorders category, which includes alcohol and drug addictions.
The decision to move gambling disorder alongside substance use disorders reflects a new understanding of the underlying commonalities between gambling and other addictions. There is a growing body of neuroscience and psychology research suggesting problem gambling is similar to drug addiction.
Many of the diagnostic criteria for gambling disorder share features with those for drug dependence, such as tolerance, withdrawal, repeated unsuccessful attempts to cut back or quit, and major interference in one's life. Problem gamblers also report cravings and highs in response to gambling.
"People will get inured to the high of gambling at a certain point and need to gamble with bigger bets and riskier betting options," says Jon Grant, who studies addiction at the University of Chicago. "When people try to stop, they go through withdrawal, with insomnia, agitation, irritability, and a feeling of being ill at ease, similar to what we see in some substance abuse disorders."
Problem gambling also runs in families, alongside other addictions. "If you have family members with alcohol use disorders, you're at increased risk for gambling disorder," says Nancy Petry, who studies addictive disorders at the University of Connecticut and served on the committee that led the reclassification of problem gambling as a behavioral addiction.
There may be some common genetic or brain differences in people who are more inclined to develop addictions, Petry says. For example, research shows that problem gamblers and drug addicts share many of the same genetic predispositions for impulsivity and reward-seeking behaviors.
This Is Your Brain on Gambling
Much of the research that supports classifying gambling disorder with other addictions comes from brain imaging studies and neurochemical tests. These have revealed commonalities in the way that gambling and drugs of abuse act on the brain, and the way the brains of addicts respond to such cues. The evidence indicates that gambling activates the brain's reward system in much the same way that a drug does.
"Across many studies, the same brain areas come up time and time again — the ventral striatum and the prefrontal cortex," says Luke Clark, a psychologist at the University of British Columbia.
The ventral striatum, located deep inside the brain, has been termed the brain's reward center, and it's been implicated in reward processing as well as substance abuse.
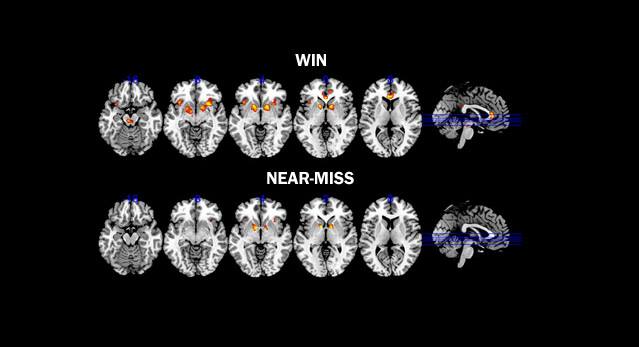
When people with gambling disorder watch gambling videos or participate in simulated gambling while their brains are being scanned, scientists can see changes in blood flow in specific brain areas, indicating which areas are more active. In one study, both problem gamblers and cocaine addicts watched videos related to their addictions while in a functional magnetic resonance imaging (fMRI) scanner. Both groups showed diminished activation in the ventral striatum compared to healthy control participants. Problem gamblers also showed less ventral striatum activity during simulated gambling games and during the anticipation of monetary rewards than did people without gambling problems.
"These results resonate with findings showing that adolescent smokers and individuals with alcohol dependence also show blunted ventral striatum activation during reward anticipation," says Marc Potenza, a psychiatrist who studies gambling addiction at the Yale School of Medicine.
While the finding that problem gamblers have lower activation in reward pathways may seem counterintuitive, some scientists think it can be explained by what’s known as the reward deficiency model. They argue that people prone to addiction have an underactive brain reward system and that such people are drawn to ways to stimulate their reward pathways, which can include the highs of drugs and gambling.
The other brain region that is often implicated in gambling and substance use disorders is the prefrontal cortex. This region is involved in decision-making, controlling impulsivity, and cognitive control. Several studies have shown that problem gamblers and drug addicts both showed less activation of the prefrontal cortex in response to gambling-related cues.
"Given the role of the prefrontal cortex in reward evaluation and delayed discounting, where people make decisions about choosing an immediate small reward versus a later, larger reward, the findings seem to suggest that individuals with gambling problems may have differences in functioning in this brain region," Potenza says.
Many studies have shown that people with gambling disorder are more impulsive than other people. They may have difficulty controlling their impulses due to reduced activation of the prefrontal cortex.
"I think the take-home message is that there are probably several types of processing problems in people with gambling disorder," Grant says. "Research indicates they are processing risk and reward incorrectly and processing current versus long-term consequences incorrectly."
Many Unknowns
Despite these studies, it is still unclear whether gambling changes the brain. "If we look at the brain of someone who has been gambling for 20 years, we definitely see differences, but cause or effect is unknown," Grant says.
People might inherently have differences in brain structure and function that lead to gambling problems, or disordered gambling could cause changes in the brain — or some combination of the two could be possible.
"We're studying the gamblers at the end of a long trajectory into their addiction," Clark says. "We need longitudinal studies about how the brain changes over time. In particular, we need to study people early in this trajectory, those who gamble recreationally but for whom it hasn't yet become a problem. We need to follow them as some escalate their gambling into high-risk behavior and others do not."
This kind of research could help identify who is at risk of developing gambling and substance abuse problems. "We need to understand what differentiates someone whose gambling is going to get worse from someone who can control their gambling," Clark says. "Those studies will shed light on whether gambling changes the brain."
Scientists who study problem gambling hope that understanding the full complexity of the underlying neuroscience will eventually help parse out individual differences in the disorder. "Neuroscience may tell us how many different types of problem gamblers there are and how we can tailor treatments for them," Grant says.
The evidence from brain studies points to many shared characteristics of gambling disorder and other addictions. Problem gamblers resemble drug addicts, not only in their behavior, but also in their brains. This has led to a new understanding of addiction: What used to be thought of as dependency on a chemical is now being defined as the repeated pursuit of a rewarding experience in spite of serious repercussions. That experience could be the high from a drug or the high of winning a bet, because behaviors can be addictive, too.
CONTENT PROVIDED BY
BrainFacts/SfN
References
DeCaria CM, Hollander E, Grossman R, Wong CM. Diagnosis, neurobiology, and treatment of pathological gambling. Journal of Clinical Psychiatry. Vol 57(Suppl 8): 80-84 (1996).
Hodgins, DC, Stea JN, Grant JE. Gambling disorders. The Lancet. 378(9806): 1874-1884 (2011).
Petry NM, Blanco C, Auriacombe M, Borges G, Bucholz K, et al. An overview of and rationale for changes proposed for pathological gambling in DSM-5. Journal of Gambling Studies. 30(2): 493-502 (2014).
Petry NM, Stinson FS, Grant BF. Comorbidity of DSM-IV pathological gambling and other psychiatric disorders: Results from the national epidemiologic survey on alcohol and related conditions. Journal of Clinical Psychiatry. 66(5): 564-574 (2005)
Potenza, M. The neurobiology of pathological gambling and drug addiction; an overview and new findings. Proceedings of the Royal Society of London B. 363: 3181-3189 (2008).
Reuter J, Raedler T, Rose M, Hand I, Gläscher J, et al. Pathological gambling is linked to reduced activation of the mesolimbic reward system. Nature Neuroscience 8: 147-148 (2005).