The Blood-Brain Barrier
- Published2 Jul 2014
- Reviewed2 Jul 2014
- Author Mary Bates
- Source BrainFacts/SfN
The brain is the only organ known to have its own security system, a network of blood vessels that allows the entry of essential nutrients while blocking other substances. Unfortunately, this barrier is so effective at protecting against the passage of foreign substances that it often prevents life-saving drugs from being able to repair the injured or diseased brain. New studies are guiding researchers toward creative ways to open this barrier and “trick” it into allowing medicines to enter.
From Hypothesis to Visual Proof
Every thought you have and action you take requires precise communication between the nerve cells in your brain. For these messages to be successfully transmitted and received, the surrounding environment needs to be stable. In the late 1800s, the surprising results of a routine test set into motion a series of experiments that revealed how the brain separates itself from the natural chemical fluctuations that occur in the body.
Mysterious Barrier
Long before German scientist Paul Ehrlich developed a cure for syphilis that would later earn him a Nobel Prize, he was fascinated by the way various tissue types absorb chemical dyes differently. Ehrlich's ultimate goal was to find new compounds that could attack disease-causing microbes. But in the course of this work, he made a strange discovery.
In 1885, Ehrlich injected blue dye into the bloodstream of mice. The dye stained all of the animals' organs blue — except their brains. In a follow-up experiment in 1913, one of Ehrlich's students injected the same dye directly into the brains of mice. This time, the brains turned blue, whereas the other organs did not.
Although these experiments suggested a physical barrier between the brain and the bloodstream, no such barrier could be detected with the instruments of the time.
An Intricate Network of Blood Vessels
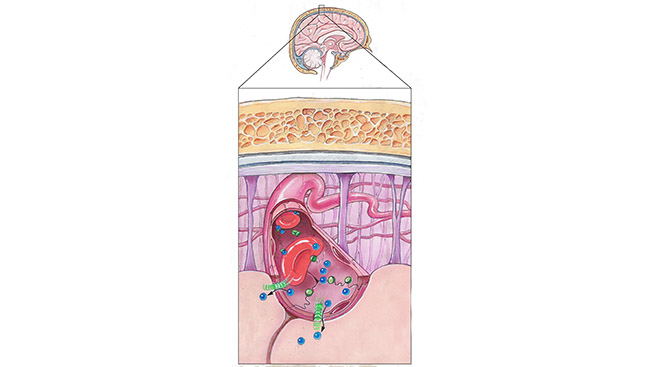
It took until the 1960s before scientists were able to catch a glimpse of the actual barrier standing between the rest of the body and the brain. Using a microscope that was roughly 5,000 times more powerful than the one Ehrlich used, scientists could see the detailed anatomy of the network of blood vessels in the brain comprising what is now known as the blood-brain barrier.
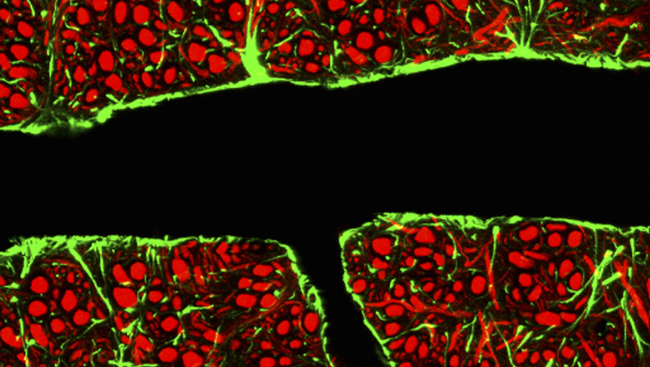
Similar to all other blood vessels in the body, scientists learned that the brain’s blood vessels are lined with endothelial cells, which serve as an interface between circulating blood and the vessel wall. However, unlike other blood vessels in the body, the endothelial cells in the brain are tightly wedged together, creating a nearly impermeable boundary between the brain and bloodstream.
Bypassing the Brain’s Barrier
The blood-brain barrier helps block harmful substances, such as toxins and bacteria from entering the brain. But, scientists knew that the brain also depends upon the delivery of hormones and key nutrients, including glucose and several amino acids, from other organs of the body.
To determine how the brain’s bouncer decides which molecules to welcome in and which to turn away, scientists injected chemicals into the bloodstreams of animals and later measured the amount that arrived in the brain.
Gaining Entry Into the Brain
Through extensive study, scientists have found that compounds that are very small and/or fat-soluble, including antidepressants, anti-anxiety medications, alcohol, cocaine, and many hormones are able to slip through the endothelial cells that make up the blood-brain barrier without much effort. In contrast, larger molecules, such as glucose or insulin, must be ferried across by proteins. These transporter proteins, located in the brain's blood vessel walls, selectively snag and pull the desired molecules from the blood into the brain.
Cells within and on either side of the blood-brain barrier are in constant communication about which molecules to let through and when. For instance, if the nerve cells in a region of the brain are working particularly hard, they will signal to the blood vessels to dilate, allowing cell-powering nutrients to quickly travel from the blood to the nerve cells in need.
Dangerous Leaks
When the blood-brain barrier breaks down, as is the case in some brain cancers and brain infections or when tiny ruptures to blood vessels occur, some substances that are normally kept out of the brain gain entry and cause problems for the brain.
Some evidence suggests the weakening of the blood-brain barrier may even precede, accelerate, or contribute to a number of neurodegenerative disorders. For instance, studies suggest a leaky blood-brain barrier allows too many white blood cells into the brains of people with multiple sclerosis (MS). With access to the brain, these cells attack myelin, the insulating coating between nerve cells, leading to the disease’s devastating symptoms.
Developing Drugs that Can Penetrate Blood-Brain Barrier
Repairing leaks in the blood-brain barrier is one hurdle for scientists. Another is determining new ways to create openings in the barrier so that life-saving drugs can access the brain.
An estimated 98 percent of potential drug treatments for brain disorders are unable to penetrate the blood-brain barrier. As a result, there are limited options for patients with brain tumors and other neurological diseases.
Barrier Crossings
In light of these challenges, researchers are now developing creative strategies to temporarily open the barrier to allow drugs to reach their targets in the brain.
One way scientists are trying to make the blood-brain barrier more permeable is by administering a solution that sucks water out of the surrounding tissues of an artery leading to the brain. This solution draws water out of the brain's endothelial cells, causing them to shrivel up, which creates gaps through which medications can temporarily pass. Within a couple hours, the cells return to normal size, closing the floodgate again.
This experimental method has been used to successfully deliver chemotherapy drugs to some patients with brain tumors. Researchers also have used this technique to temporarily create gaps in the barrier through which they can thread a microcatheter to deliver anticlotting drugs following a stroke.
Scientists are also developing new strategies for attaching drugs to molecules naturally transported across the barrier. This so-called “Trojan horse” method has shown success in several animal models by enabling drugs otherwise shut out of the brain to get in without adverse effects. However, experts caution such a technique has yet to be tested in clinical trials.
Through the development of new brain technologies, scientists are creating new ways to free up the blood-brain barrier so that life-saving drugs can reach specific targets in the brain without interfering with ongoing activity. Although numerous challenges likely lie ahead, many scientists are hopeful that new knowledge of blood-brain barrier function under normal and diseased conditions will one day lead to better treatments for some of the most challenging and intractable brain diseases.
CONTENT PROVIDED BY
BrainFacts/SfN
References
Hawkins BT, Davis TP. The blood-brain barrier/neurovascular unit in health and disease. Pharmacological Reviews. 57:173-185 (2005).
Marquet F, Tung Y, Teichert T, Ferrera VP, Konofagou EE. Noninvasive, transient and selective blood-brain barrier opening in non-human primates in vivo. PLoS One. 6(7): e22598 (2011).
Neuwelt EA, Bauer B, Fahlke C, Fricker G, Iadecola C, et al. Engaging neuroscience to advance translational research in brain barrier biology. Nature Reviews Neuroscience. 12(3): 169-182 (2011).
Palmer AM. The blood-brain barrier. Neurobiology of Disease. 37: 1-2. (2010).
Pardridge WM. Drug and gene targeting to the brain with molecular Trojan horses. Nature Reviews Drug Discovery. 1: 131-139 (2002).
Zlokovic BV. The blood-brain barrier in health and chronic neurodegenerative disorders. Neuron. 57: 178-201 (2008).