The Gut and Brain: A Surprising Connection
- Published25 Jan 2024
- Source BrainFacts/SfN
The nervous and digestive systems are in constant communication, influencing each other in some unexpected ways. Scientists estimate the gut produces over 90% of our body’s serotonin. And researchers have found bacteria in our gut can help shape a healthy stress response and maintain memory. The scientific world is beginning to unravel the relationship between the microbiome, gut health, and the brain. But what they’ve learned so far promises new ways of treating age-old problems.
This is a video from the 2023 Brain Awareness Video Contest.
Created by Diya Patel.
CONTENT PROVIDED BY
BrainFacts/SfN
Transcript
In fact, a poor gut microbiome is a risk factor for obesity, type two diabetes, and several types of cancer. But recently, neuroscientists have found that the gut also has a profound impact on our brain. The connection between our brain, gut, and its microbiome is called the gut-brain axis, or GBA for short. This is a bi-directional link, meaning it goes both ways, between our central nervous system and the enteric nervous system.
The central nervous system is made up of the brain and the spinal cord, and the enteric nervous system is the web of sensory neurons, motor neurons, and interneurons embedded in the wall of the gastrointestinal system.
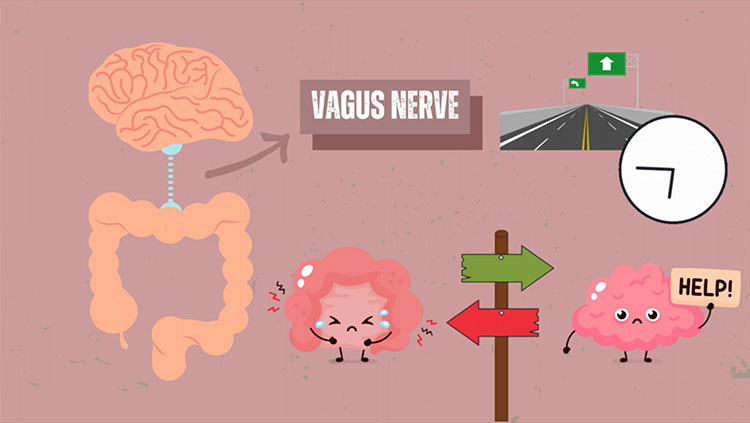
The CNS and the ENS communicate via the bidirectional link through many channels and pathways, but the vagus nerve is the primary method of communication between the brain and the gut. The sensory receptors in the ENS can pick up on cues about the gut, such as nutrient availability, microbial composition, and the presence of inflammatory molecules. These signals travel up through the vagus nerve and reach the brain.
There, the brain can modulate and monitor gut function. For example, if the brain detects irritation in the gut, it can activate motor fibers of the vagus nerve to initiate the vomiting reflex. In addition to the bidirectional communication link, the gut can influence the emotions and memory of the brain.
Bacteria in the gut can produce metabolites that directly or indirectly affect the hypothalamic-pituitary-adrenal axis or HPA axis. The HPA axis is the main stress response system of the brain. Because the gut impacts the HPA axis, it can influence the release of stress hormones such as cortisol. In fact, certain bacteria in the gut, like lactobacillus and bifidobacterium, can produce GABA: a neurotransmitter that sets the baseline for stress response of the HPA axis. But GABA is also involveds in influencing memory through synaptic plasticity.
Synaptic plasticity refers to the ability of neurons to modify the strength of their connections with each other, which is an important factor in forming memories. So, a healthy gut microbiome that can produce the right amount of GABA can result in a healthy stress response system and a strong memory.
The gut can also produce a neurotransmitter called serotonin, which is involved in mood regulation. In fact, about 90% of serotonin is produced in the gut. This means that the microbiome of the gut impacts the amount of serotonin released. The presence of some bacteria can increase serotonin levels, while the removal of some bacteria can decrease serotonin levels. So, alterations to the gut microbiome, also known as dysbiosis, have been associated with mood disorders like depression and bipolar disorders.
Lastly, the gut-brain axis also modulates inflammatory response. Dysbiosis can cause the immune system to release increased levels of pro-inflammatory factors. These same pro-inflammatory factors activate microglia and mast cells in the brain, and a chain reaction occurs that can result in the disruption of normal brain development, especially in the case of young children, and it can potentially lead to the expression of autistic traits.
Elevated levels of inflammation are also associated with cognitive decline and impaired memory. Later on in life, the inflammation can trigger proteins in the brain to clump together leading to neurodegeneration and diseases like Alzheimer's. While our understanding of the gut-brain axis has expanded significantly in recent years, since we now know how important it is for mood and stress regulation, memory, cognition, and overall wellbeing, there's still much to be learned about the gut-brain axis and its implications on human health. Additionally, exploring therapeutic strategies like the use of probiotics that target the gut-brain axis holdholds promise for managing and treating various conditions like anxiety, depression, and autism. Continued research into this fascinating field will undoubtedly result in more therapies to treat disorders in ways we never thought possible before.