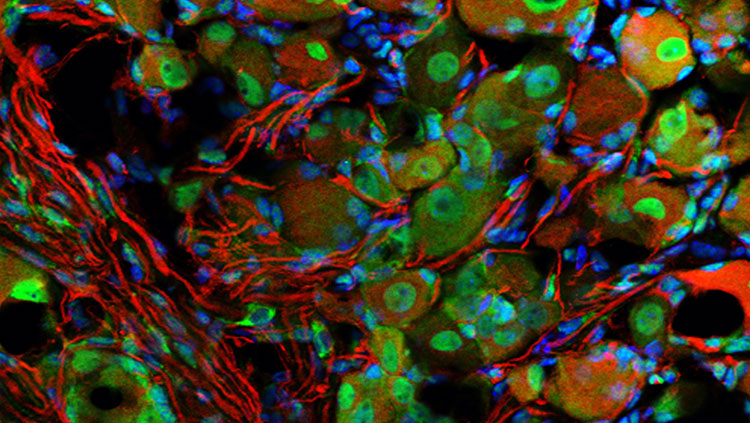
A migraine is not a run-of-the-mill headache. Pain-sensing neurons, called nociceptors, around the brain’s blood vessels appear to play a key role. Rhode Island School of Design student Peyton North created this video with Phoebe Draper and Jeff Wu to illustrate what happens in the brain when a migraine occurs. While neuroscientists are still studying this process, they think that migraines result from an overly sensitive pain pathway from these nociceptors. This video was submitted for the 2014 Brain Awareness Video Contest.
Migraines are much more than just headaches. A migraine is preceded by strange sensations and peculiar brain activity. The extreme pain that ensues is a result of activation of receptors and blood vessels outside the brain feeding into an overly sensitive pain pathway within the brain. Let’s look at these aspects in greater detail. It is generally accepted that changes in the blood flow to vessels surrounding the brain are associated with migraine pain. The walls of blood vessels are lined with sensory neurons called nociceptors. When blood flow in the head changes, these nociceptors are activated and send an electrical message to the brain that is interpreted as pain. But changes in blood flow happen all the time and don’t always lead to a migraine. There has to be more to the story. Recent theories propose that the trigemino-vascular pain pathway - brain wiring that connects blood vessels to the part of the brain that processes pain - is the major player. In migrainers, this pathway is overly sensitized, so stimuli like stress, exercising, and certain foods that don’t usually trigger pain activate the pain pathway. There are other migraine symptoms, known as auras, that seem to have nothing to do with the pain pathway. Often, migraines report one part of their vision becoming blurry - the blurriness slowly spreading to more distant parts of their visual field. The timing of this visual disturbance perfectly matches that of a well-characterized electrical disturbance called cortical spreading depression. This abnormal wave of electrical activity marches across the brain at about five millimeters per minute. When it invades the occipital lobe, it affects vision. If it marches over the parietal lobe, it affects sense of touch and illicits a tingling sensation. Beyond pain and aura, migraine symptoms are numerous and vary among sufferers. It is difficult for researchers to pin down a unifying explanation. Strings of commonality have allowed us to piece together what we do know. That nociceptors and blood vessels outside the brain are part of the story and sensitization of pain pathways may be the condition that predisposes people to migraines. However, scientists are still searching for answers as to why some people are wracked with migraines daily while others may never experience one.