Animal Research Success: Psychiatric Disorders
- Published9 Mar 2012
- Reviewed9 Mar 2012
- Author Emily K. Dilger, PhD
- Source BrainFacts/SfN
The discovery of new medications to treat psychiatric disorders requires the ability to identify promising new chemical compounds and weed out less effective ones. This can be accomplished by setting up screening procedures that predict the effectiveness of different compounds in patients.
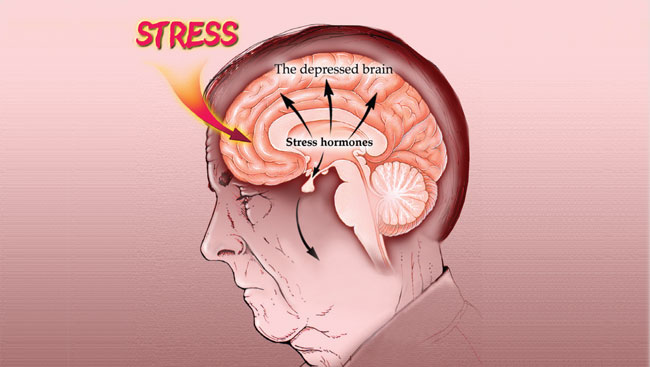
Brain system malfunctions can result in various psychiatric disorders, such as depression. Physical symptoms, including difficulty sleeping and loss of appetite, probably result from excessive production of stress hormones.
Since the 1950s, animal models have been central to the discovery of drug treatments for such serious disorders as depression, anxiety disorders, and schizophrenia. The most efficient and useful screening procedures involved testing medications with rats and mice and observing their effects on specific, well-characterized behaviors. Tests of anxiety and anxiolytic drugs are examples of the successful use of screening procedures.
Here's how it works: Rats and mice avoid predators, such as birds of prey, by favoring dark, enclosed spaces over open ones. However, these animals must occasionally venture into light, uncovered spaces to obtain food. The balance between how much time a rat or mouse spends in dark versus light spaces has been used to identify many anxiolytic drugs. While there are many specific versions of such tests, the major theme is that drugs that increase the proportion of time that a rodent is willing to spend in the open is a good predictor of relief of anxiety symptoms in human patients.
Despite progress in developing treatments for many psychiatric disorders, our understanding of what goes wrong in the brain remains incomplete. One important set of clues is that disorders such as autism, schizophrenia, and bipolar disorder are highly influenced by genes. The genetic contribution to these illnesses is complicated, with many genes contributing to risk along with environmental factors.
In a small number of families affected by autism or schizophrenia, however, a single genetic mutation may cause the disorder. Animal models are important in helping scientists understand how these genetically based disease risks produce symptoms. It is now possible to replace a mouse gene with the equivalent human gene associated with disease. For example, in some cases in which autism appears to be caused by a single gene, the human gene has been inserted inside a group of experimental mice, replacing their original mouse gene. Interestingly, the mice exhibit behaviors highly reminiscent of human autism. Depending on the precise gene that has been tested, the mice with the human gene may avoid social interactions with other mice, engage in repetitive behaviors, or both.
Scientists then use such mice to search for causes for the brain abnormalities. The ultimate goal is not only to understand the disease processes, but also to gain clues for the development of new, effective treatments. It is still early days in human gene identification and in the creation of genetic mouse models of brain disorders, but this approach is showing enormous promise.
One of the challenges of brain research is that this highly complex organ contains thousands of distinct types of neurons, which give rise to many complex circuits. A new technique that has powerful implications for understanding brain disorders permits us to manipulate individual types of cells and circuits. This technology, called optogenetics, involves the insertion of genes into particular neurons in the brains of mice. These genes cause the neurons to fire in response to specific colors of light, providing information about the cellular changes that arise as a result. This new technology has already contributed to the analysis of many circuits that play a role in normal thought and emotions, as well as in brain disorders.
CONTENT PROVIDED BY
BrainFacts/SfN
Also In Archives
Trending
Popular articles on BrainFacts.org