Restoring Vision in Older Adults Can Reduce Risk of Dementia
- Published30 Jun 2022
- Author Zunnash Khan
- Source BrainFacts/SfN
Without question, cataract surgery can restore clouded vision by removing the eye’s milky lens and replacing it with a clear, artificial one. What hasn’t been so obvious is the potential for cataract surgery to preserve cognitive functioning in older adults.
A study published in Journal of the American Medical Association Internal Medicine shows people who received cataract surgery reduced their risk for dementia by nearly 30%. The findings hint at the importance of visual stimulation for cognitive health.
“The paper established that loss of vision has a role in cognitive impairment,” says Joshua Ehrlich, an ophthalmologist at the University of Michigan, about the study led by Cecilia Lee. Lee, a retina specialist and clinical epidemiologist from the University of Washington, had begun exploring the connection between visual acuity and cognitive health because she was interested in whether the retina could be a biomarker of cognitive disease.
Making the Most of Medical Records
Cataracts arise when proteins in the lens degrade and clump as we age. To study the effect of removing these clouded lenses, Lee made use of a collaboration with the Adult Changes in Thought (ACT) study. The longitudinal ACT study began in 1994 and aims to identify dementia risk factors in people by analyzing their medical records. Every two years, study participants undergo screening with an extensive cognitive evaluation tool known as the Cognitive Abilities Screening Instrument (CASI). Screening scores range from 0 to 100, with higher scores indicating more functional cognitive abilities. Participants scoring below 85 receive further testing to determine whether they meet the criteria for a dementia diagnosis.
Lee’s team analyzed ACT participant data, examining those who were 65 or older and dementia-free at the start of the study until they developed dementia or passed away. By studying records of around 3000 participants from 1994 to 2018, she concluded cataract surgery reduced the risk of dementia in the study population by 29%.
Because cataract surgery is an elective outpatient procedure, any patient who undergoes it may be healthier at the baseline and at a lower risk of developing dementia. To test whether the link between cataract surgery and cognitive health arose from healthier people undertaking the procedure, known as the healthy patient bias, Lee analyzed the data for another generally elective outpatient surgery: glaucoma. Glaucoma is damage to the optic nerve most often caused from fluid buildup in the eye that causes high pressure and loss of vision. Glaucoma surgery is performed to reduce the pressure in the eye, but it doesn’t restore vision. “Patients should have had a similar health [baseline] to undergo glaucoma surgery” as they did for cataract surgery, Lee said. However, she didn’t find any association between dementia and glaucoma surgery.
Lee concluded the reduced risk of dementia from cataract surgery is related to the improvement in vision and that patients were healthy enough to undergo any eye surgery.
Looking for More Clues
Ehrlich notes vision loss can lead to a more isolated and confined lifestyle, and social isolation is a known risk factor for dementia. Not being able to engage in cognitively stimulating social activities or take up hobbies like reading, solving puzzles, and board games due to vision loss can accelerate cognitive decline. A lack of visual stimulation could also translate into reduced brain stimuli, thereby affecting cognition.
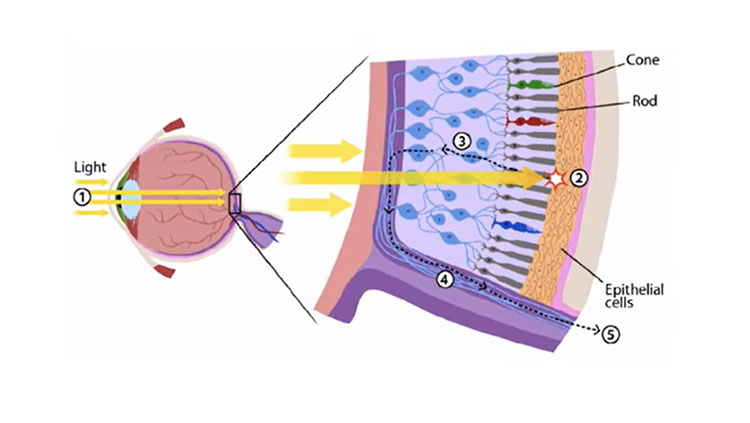
Lee even suspects a possible mechanism. Cataracts have a yellowish hue that filters blue wavelength from the natural light entering the eye. “There’s a special population of ganglion cells in the retina of the eye that are known to regulate our sleep cycles, circadian rhythms, and are also potentially associated with cognition and mood. And we know that they get stimulation with blue light,” she explained. When the cataract is extracted, people see more blue light which improves stimulation of these cells. This could play a role in improving cognitive function.
Although Lee looked at dementia-free adults in her study, she noted some literature “suggests that cataracts surgery may also be important in patients who already have dementia,” expressing hope that if her finding is validated by future studies, eyecare can be used as a strong healthcare measure for older people at risk of dementia.
CONTENT PROVIDED BY
BrainFacts/SfN
References
Adult Changes in Thought (ACT) Study. Kaiser Permanente Research. https://actagingresearch.org/about/research-program
Cataracts. (2021). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/cataracts/symptoms-causes/syc-20353790
Cataract Surgery. (2021). Mayo Clinic. https://www.mayoclinic.org/tests-procedures/cataract-surgery/about/pac-20384765
Lee, C.S., Gibbons, L.E., Lee, A.Y., Yanagihara, R.T., Blazes, M.S., Lee, M.L., McCurry, S.M., Bowen, J.D., McCormick, W.C., Crane, P.K., Larson, E.B. (2021). Association Between Cataract Extraction and Development of Dementia. JAMA Internal Medicine, 182(2), 99-239. https://doi:10.1001/jamainternmed.2021.6990
Girard, B., Chouard, B., Levy, P., Luquel, L., Seux, M. L., & Drunat, O. (2016). Modifications des troubles du comportement après l’opération de la cataracte chez les patients Alzheimer [Neuropsychological benefit of cataract surgery among sight impaired Alzheimer's patient]. Journal francais d'ophtalmologie, 39(8), 675–686. https://doi.org/10.1016/j.jfo.2016.05.005
Glaucoma. (2022). National Eye Institute. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma
Glaucoma Surgery. (2022). National Eye Institute. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma/glaucoma-surgery
Shrank, W. H., Patrick, A. R., & Brookhart, M. A. (2011). Healthy user and related biases in observational studies of preventive interventions: a primer for physicians. Journal of general internal medicine, 26(5), 546–550. https://doi.org/10.1007/s11606-010-1609-1
Teng, E.L., Hasegawa, K., Homma, A., Imai, Y., Larson, E., Graves, A., Sugimoto, K., Yamaguchi, T., Sasaki, H., Chiu, D., et al. (1994). The Cognitive Abilities Screening Instrument (CASI): a practical test for cross-cultural epidemiological studies of dementia. International Psychogeriatrics, 6(1):45-58. https://doi.org/10.1017/S1041610294001602