Dopamine and Movement
- Published22 Oct 2015
- Reviewed7 Oct 2015
- Author Susan Perry
- Source BrainFacts/SfN
Dopamine is a messenger molecule in the brain that allows certain nerve cells to communicate with one another. Underestimated at its discovery, dopamine proved critical to central nervous system functions such as movement, pleasure, attention, mood, and motivation. Discovering dopamine’s role in Parkinson’s disease changed the field of neuroscience and led to a profound breakthrough in the treatment of the disease.
A central role in cell communication
While today it is recognized as a crucial part of brain function, scientists did not immediately recognize dopamine’s importance when it was first discovered in the brain in the early 1950s. Dopamine bears a striking resemblance to another naturally occurring chemical prevalent throughout the nervous system, norepinephrine. As such, scientists thought it was a simple building block for the production of norepinephrine.
In addition, at the time it wasn’t clear that chemicals played a role in transferring information between brain cells (neurons). While scientists had demonstrated that nerves outside of the brain communicate with muscles and organs via chemical messengers, there was little evidence to suggest that these chemical messengers were also used in the brain, and many scientists insisted that brain cells communicated only via electrical impulses.
An Unexpected Finding
The evidence for dopamine signaling in the brain came from experiments conducted in 1957 by a young Swedish pharmacologist named Arvid Carlsson. Carlsson studied rabbits exposed to high doses of the drug reserpine, which depletes stores of norepinephrine and leaves the animals rigid and immobile. Carlsson wanted to see whether injecting levodopa (L-dopa), a chemical the brain converts into dopamine, directly into the rabbits’ brains would restore movement by ultimately replenishing norepinephrine. It worked. The rabbits recovered. However, the animals’ brains contained little norepinephrine. Instead, Carlsson found the brains awash in dopamine.
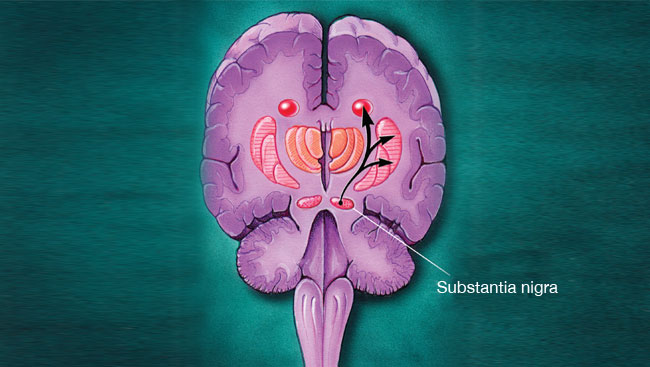
After developing a new technique to measure dopamine, Carlsson and his colleagues discovered that an area of the rabbit brain called the striatum housed high concentrations of dopamine under normal conditions despite the fact that it had very little norepinephrine. The striatum is one of the structures that make up the basal ganglia, a group of brain structures that scientists had identified as important in Parkinson’s disease. The debilitating tremors, muscle rigidity, and decreased ability to move that are associated with Parkinson’s disease reminded Carlsson of the reserpine-triggered symptoms in rabbits.
Carlsson proposed that Parkinson’s disease arose from the degeneration of dopamine-containing cells in the basal ganglia. It was a radical idea — it went against the prevailing theory of electrical neural transmission in the brain and suggested that some brain cells used dopamine to communicate.
A treatment breakthrough
Soon after Carlsson published his seminal papers in 1957 and 1958, other researchers reported the presence of large quantities of dopamine in the basal ganglia of normal human brains. Austrian pharmacologist Oleh Hornykiewicz found substantially lower dopamine levels in the basal ganglia of people who had died with Parkinson’s disease. Today, it is generally recognized that the tremor and other symptoms of Parkinson’s disease arise from the death of dopamine-producing cells in the basal ganglia — just as Carlsson had predicted.
A Dramatic Reversal of Symptoms
In 1961, Hornykiewicz, working with neurologist Walter Birkmayer, gave intravenous L-dopa to 20 volunteers with Parkinson’s disease. The results were dramatic: L-dopa treatment restored the ability of patients with severe Parkinson’s disease to resume normal movement for up to 24 hours. Patients who had been immobile and bedridden not only sat up, but could stand and walk. Some even ran and jumped. The drug also allowed some patients to speak normally for the first time in years.
Unfortunately, treatment with L-dopa frequently caused severe nausea and vomiting, limiting its practical use. In 1967, scientist George Cotzias figured out that slowly increasing the drug’s dosage allowed the patient to adjust to a dose that could effectively alleviate symptoms of Parkinson’s disease without severe side effects.
In 1970, the U.S. Food and Drug Administration approved L-dopa for the treatment of Parkinson’s disease. However, L-dopa is not a cure. In some patients, the doses of L-dopa needed to move cause involuntary movements (“dyskinesia”). Still, L-dopa revolutionized the treatment of Parkinson’s disease, enabling millions of people to lead more normal lives. Almost half a century later, the drug remains the most common and effective treatment of the disease.
A deeper understanding of dopamine’s role in the brain
The 1970s saw an explosion of dopamine research as scientists tried to understand exactly how it exerts its influence in the nervous system. American neuroscientist Paul Greengard conducted a series of groundbreaking experiments describing how dopamine works: By attaching to multiple receptors on the surface of a neuron, dopamine initiates different chains of chemical reactions that alter the function of the nerve cell, including its ability to send impulses to other neurons.
Beyond Parkinson’s
Dopamine is now known to play many roles in the brain, and the dysfunction of brain circuits that use dopamine is involved in the development of not just Parkinson’s disease, but many other neurological and psychiatric disorders. These include other movement disorders, such as Huntington’s disease, as well as depression, anxiety disorders, schizophrenia, obsessive-compulsive disorder, and attention deficit hyperactivity disorder (ADHD).
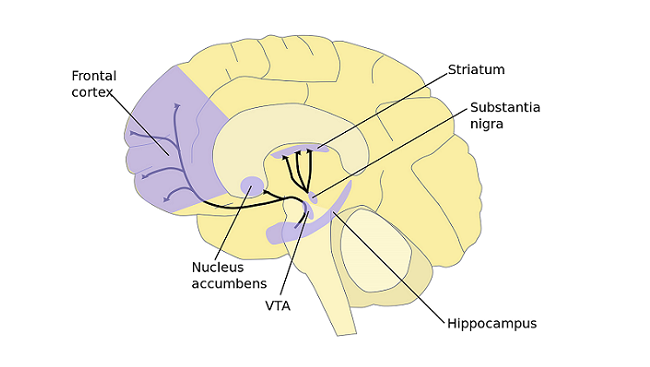
Both depression and anxiety have been linked to inactive dopamine receptors in the nucleus accumbens, an area within the basal ganglia that is associated with pleasure and reward. Researchers have also found that overactive dopamine pathways — ones that flood the brain with too much, rather than too little, of the neurotransmitter — are involved in several neuropsychiatric disorders, including schizophrenia and drug addiction.
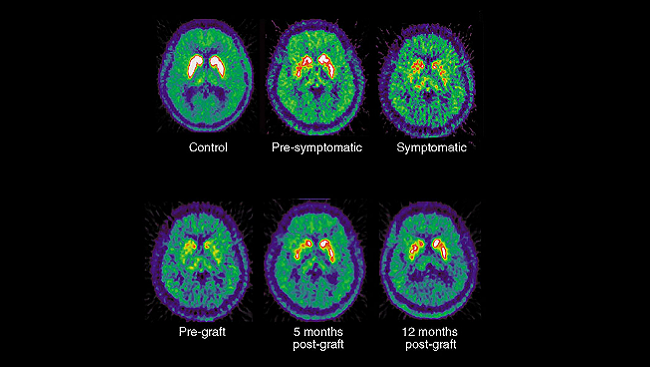
These findings have led to many new treatment possibilities for psychiatric and behavioral disorders; scientists continue to study dopaminergic circuits to continually improve on these treatments. For example, with optogenetics, light-sensitive proteins are implanted into neurons, enabling them to be controlled with light, and this technology could potentially be used to activate the pathways that dopamine fails to act on or silence overactive dopamine pathways.
More than half a century after the discovery of dopamine’s role in Parkinson’s disease, dopamine continues to reveal its molecular mysteries. With the help of research funded by private and public institutions, scientists continue to advance our understanding of dopamine’s complex role in the brain and offer hope to the millions of people around the world suffering from dopamine-related diseases.
CONTENT PROVIDED BY
BrainFacts/SfN